What is Gum Disease?
Gum or periodontal disease is a common condition affecting the gums and the supporting tissues of the teeth. It is caused by plaque buildup on the teeth and gums, which can lead to infection and inflammation.
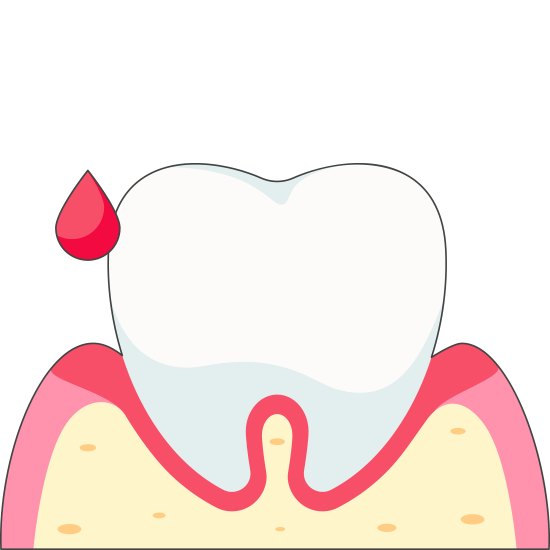
Gingivitis is the early stage of gum disease, characterised by red, swollen, and bleeding gums.
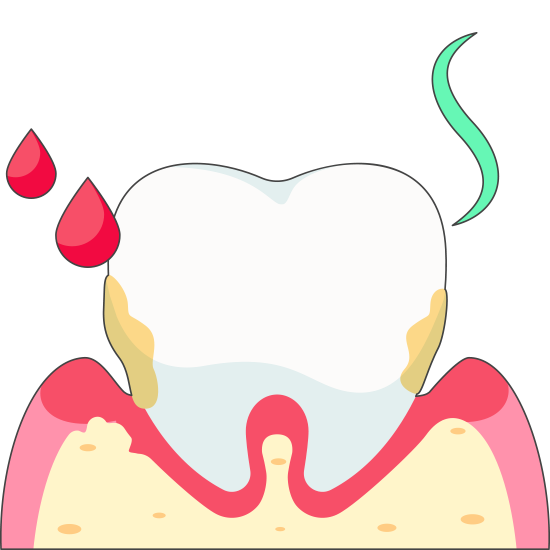
When left untreated, gingivitis can progress to periodontitis, a more severe form of gum disease that can cause the gums to recede and pull away from the teeth, creating pockets where bacteria can accumulate and cause infection.
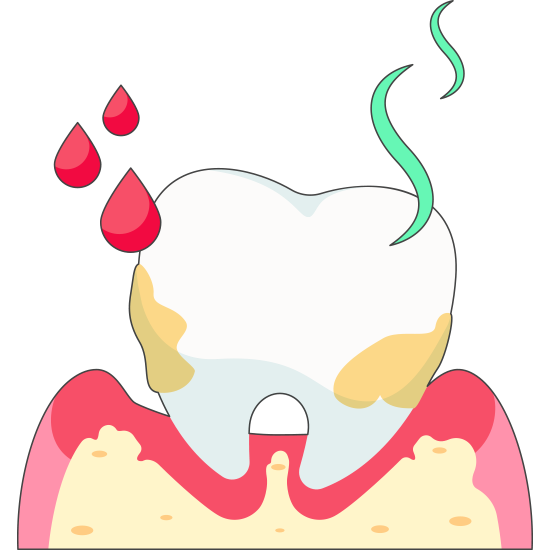
If periodontitis is left untreated, it can lead to tooth loss and damage to the bone and other structures that support the teeth.
Some common symptoms of gum disease include:
- Red, swollen, or tender gums
- Bleeding gums, especially when brushing or flossing
- Receding gums
- Persistent bad breath
- Loose teeth or changes in the way teeth fit together
- Pain or sensitivity in the teeth
Gum disease can be prevented through good oral hygiene practices, including regular brushing and flossing, using an antiseptic mouthwash, and visiting the dentist for regular checkups and cleans.
Gum disease treatment typically involves deep cleaning of the teeth and gums to remove plaque and bacteria.
In more severe cases, surgery may be necessary to repair damaged tissues and prevent tooth loss.
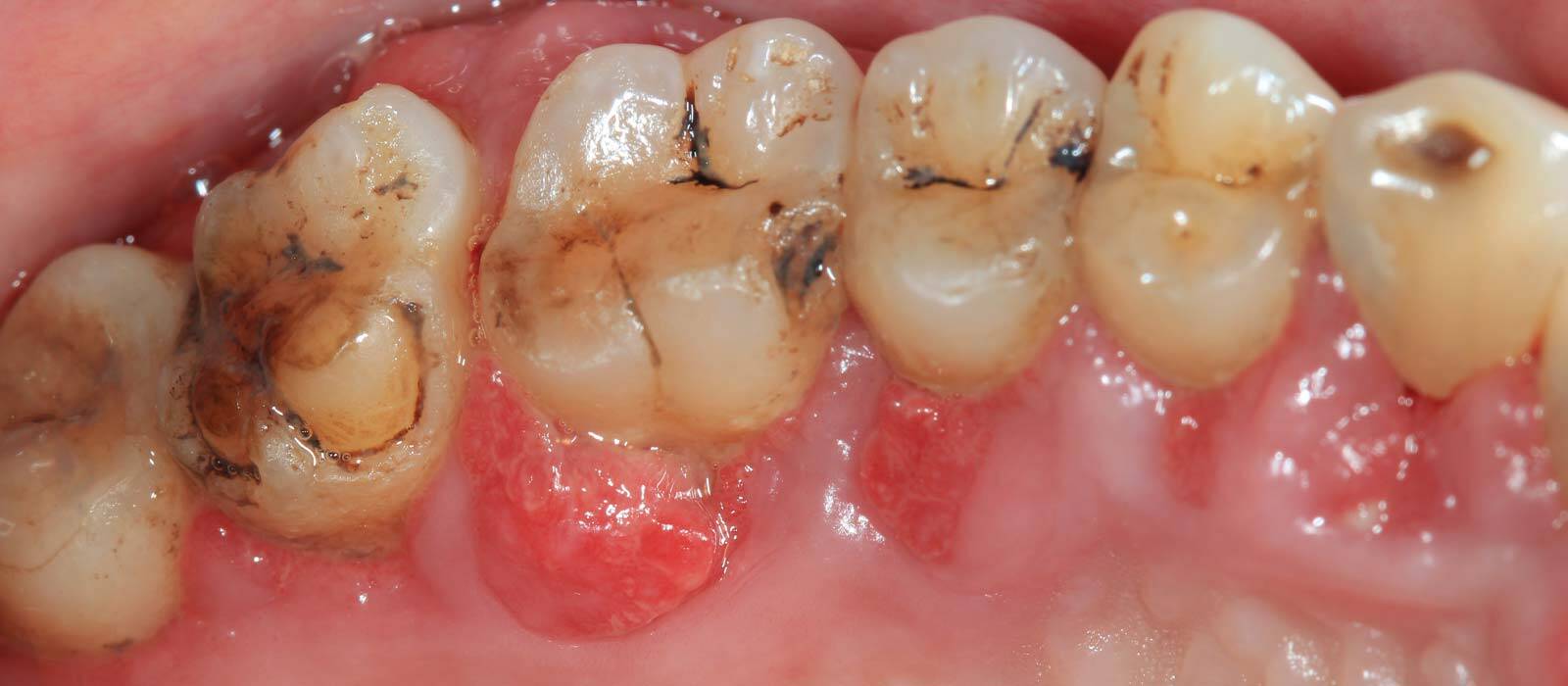
We help to protect & prevent your teeth from Periodontitis
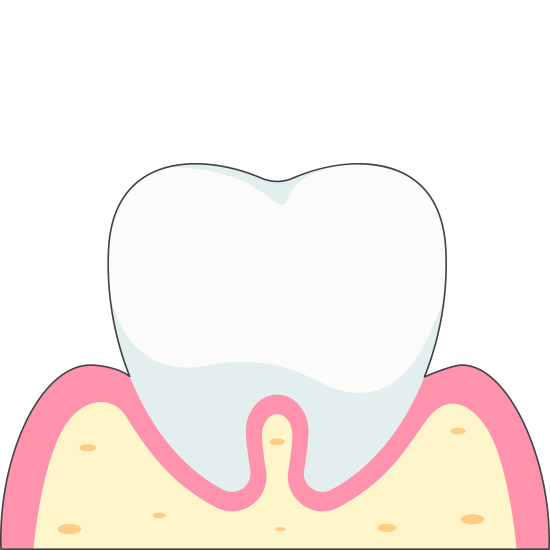
Stages of Gum Disease
Periodontitis is a dental disease caused by bacterial infections that impacts the gums and bone supporting the teeth. It begins with gingivitis and progresses through moderate to advanced stages. Each stage has distinct symptoms and necessitates specific treatments.
In summary, Periodontitis is a progressive oral disease that develops in stages, starting with normal teeth and progressing to gingivitis, moderate periodontitis, and advanced periodontitis. Each stage of the disease has different symptoms and requires different treatments.
Maintaining good oral hygiene practices, such as regular brushing and flossing, and visiting the dentist regularly to detect and treat Periodontitis early is essential.
With proper treatment, the progression of Periodontitis can be slowed or even stopped, and the health of the gums and teeth can be maintained.
How to treat Gingivitis?
General dentists can diagnose and treat gingivitis, the initial stage of gum disease. The primary treatment is removing plaque and tartar through scaling and root planing, which cleans the teeth and gums of harmful bacteria. Dentists may also suggest antiseptic mouthwash to help control bacteria and promote healing.
Additionally, they provide guidance on good oral hygiene practices, like proper brushing and flossing, to prevent future buildup. Regular dental checkups and cleanings are crucial for preventing gum disease and other oral health issues.
If you notice symptoms like red, swollen, or bleeding gums, seek dental treatment promptly to avoid more serious problems. In severe cases of gum disease, you may be referred to a specialist called a periodontist.
Treating Periodontitis
Treatment for advanced periodontitis involves a multi-step process to eliminate the infection and prevent further damage to the gums and bone.
Here are the typical steps involved in treating advanced periodontitis:
- Scaling and Root Planing: The first step in treating advanced periodontitis is a deep cleaning called scaling and root planing. This removes plaque and tartar from teeth and below the gum line using special instruments.
- Gum Surgery: Gum surgery may be recommended if the condition doesn’t improve after deep cleaning. This involves removing infected tissue and reshaping the gums. Types of gum surgery include flap surgery and bone grafting.
- Antibiotic Therapy: To help eliminate infection-causing bacteria, antibiotics may be prescribed alongside other treatments, either orally or applied directly to the gums.
- Ongoing Maintenance: After initial treatment, A strict oral hygiene routine is essential. This includes regular dental checkups, daily brushing and flossing, and using special mouthwashes.
In severe cases, tooth extraction might be necessary, and dental implants or other replacements can be discussed.
Advanced periodontitis requires immediate and thorough treatment to prevent tooth loss. This includes deep cleaning, potential gum surgery, antibiotics, and diligent maintenance for optimal oral health. Patients should collaborate with their dentist or periodontist to create a tailored treatment plan.
Get Started with a Check-Up & Clean
Regular dental check-ups and cleans are essential for keeping your teeth and gums healthy and preventing gum disease.
Gum disease is common and can seriously harm your teeth and gums if not treated. Symptoms like bleeding or swollen gums may go unnoticed until late.
By visiting your dentist for a check-up and clean, they can spot any signs of gum disease and create a treatment plan to stop further damage. Please don’t wait until it’s too late. Take care of your oral health, book a dental check-up, and clean today.
FAQ’s
Does private health insurance cover gum disease treatment?
Private health insurance policies differ in dental coverage, including gum disease treatment. Coverage may be part of ‘extras’ or ‘hospital’ policies. Some plans may entirely or partially cover treatments like scaling, root planning, or periodontal surgery, while others may not.
Always check your policy details for coverage, limitations, and exclusions. Be aware of waiting periods, annual limits, and gap fees associated with dental treatments.
Contact an Amazing Smiles Dental Clinic near you for questions about your coverage.
Do I need to see a specialist for Periodontal disease?
A general dentist can handle basic periodontal disease treatments like scaling and root planing. However, for advanced or severe gum disease, you may need to see a periodontist, a specialist trained in diagnosing and treating these conditions, and placing dental implants.
Periodontists are equipped to manage complex cases or those that haven’t improved with initial treatment. Your general dentist can evaluate your condition and refer you to a periodontist if necessary. Reasons for seeking a specialist include:
- Advanced or severe periodontal disease
- Complex treatment needs
- Gum grafting or bone regeneration requirements
- Underlying health issues that complicate treatment
Ultimately, whether to see a periodontist will depend on your specific situation and your dentist’s advice. Remember that periodontists focus solely on gum health and do not handle general or cosmetic dental needs.
Do I need a crown or dental implant after root canal therapy?
Whether you need a crown or a dental implant after a root canal depends on the condition and location of your tooth, along with your overall dental health. After a root canal, the tooth may be weakened and more prone to fractures, often requiring a crown to protect it and restore its strength and appearance.
If the tooth’s damage is severe and a crown isn’t sufficient, a dental implant may be necessary. This involves placing an artificial tooth root into the jawbone, followed by a crown or other restoration.
Your dentist will assess your situation and determine whether a crown or an implant is the best option for your needs.
We accept all major health funds

Make an Enquiry
We are proud to be preferred providers with most major health funds, allowing our patients to maximise their health cover benefits and access quality care at greater value. To make treatment more accessible, we also offer a variety of flexible payment plans to help individuals manage the cost of their dental care in a way that best suits their financial situation.
Start your journey toward a healthier, more confident smile by booking your complimentary smile consultation with Amazing Smiles today.