Table of Contents
Dry mouth, medically known as xerostomia, is a common oral health condition that affects many individuals.
It occurs when the salivary glands do not produce enough saliva, leading to a dry and uncomfortable sensation in the mouth.
A dry mouth can significantly impact oral health, causing problems such as tooth decay, bad breath, and difficulty speaking and swallowing.
Causes of Dry Mouth
Occasionally, dry mouth can occur due to a condition directly affecting the salivary glands, which produce saliva. Saliva plays a crucial role in maintaining good oral health.
It helps protect our teeth by neutralising the acids produced by bacteria, reducing bacterial growth, and rinsing away food particles.
Saliva also contributes to our ability to taste, making our meals more enjoyable.
It aids in chewing and swallowing, and the enzymes present in saliva assist in the digestion of food.
Having less saliva and experiencing dry mouth can vary from being a minor inconvenience to significantly affecting your overall health and the health of your teeth and gums. It can also impact your appetite and enjoyment of food.
Certain medications, such as antidepressants, antihistamines, and diuretics, can decrease saliva production.
Medical conditions like Diabetes, Sjögren’s Syndrome, and Parkinson’s Disease can also contribute to dry mouth. Habits like smoking and excessive alcohol consumption can worsen the condition, and saliva production naturally decreases as we age.
Various factors can cause a dry mouth. These can include:
- Medications: Certain medications, such as antidepressants, antihistamines, and diuretics, can reduce saliva production and lead to dry mouth.
- Dehydration: Not drinking enough water or experiencing excessive sweating, vomiting, or diarrhea can result in dehydration and dry mouth.
- Smoking and Alcohol: Tobacco use and excessive alcohol consumption can contribute to dry mouth as they can affect saliva production.
- Medical Conditions: Several conditions, including Diabetes, Sjögren’s Syndrome, HIV/AIDS, and Parkinson’s Disease, can cause dry mouth.
- Nerve Damage: Injuries or surgeries that affect the head and neck area can damage the nerves responsible for saliva production, leading to dry mouth.
- Aging: As we age, salivary glands may become less efficient, resulting in decreased saliva production and dry mouth.
- Hormonal Changes: Hormonal changes during pregnancy or menopause can disrupt the normal functioning of the salivary glands, leading to a decrease in saliva production. This hormonal imbalance can result in a dry mouth, making it more difficult to speak, chew, swallow, and maintain oral health.
Symptoms of xerostomia

Recognising the symptoms of dry mouth is crucial for early detection and prompt treatment. Common signs include:
- A persistent dry or sticky saliva feeling in the mouth
- Frequent thirst
- A sore throat
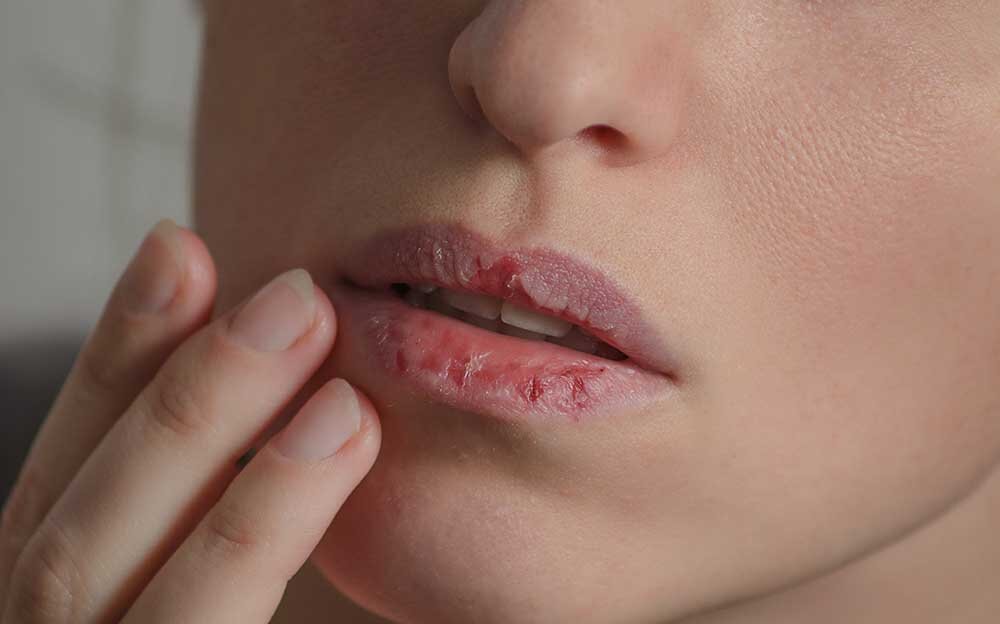
- Cracked lips
- Difficulty speaking, chewing, and swallowing
- Wearing dentures
- Altered sense of taste
- Bad breath
If you experience these symptoms, it is essential to consult a dental professional or healthcare provider for an accurate diagnosis and appropriate management.
Self-care Home Remedies for Dry Mouth
While it’s essential to consult a healthcare professional for proper diagnosis and treatment, several home remedies can help alleviate dry mouth symptoms. Staying hydrated and drinking plenty of water throughout the day is also crucial.
Chewing sugar-free gum or sucking on sugar-free candies can stimulate saliva flow. Avoiding caffeine, alcohol, and tobacco products can also help. A humidifier in your bedroom can add moisture to the air and relieve dryness.
Dental or Medical Treatment Solutions
If you are experiencing ongoing signs and symptoms of dry mouth, you should schedule an appointment with a healthcare professional.
When home remedies aren’t enough, it’s important to seek professional in-person advice to address the underlying causes of dry mouth. Dry mouth requires a comprehensive approach focusing on symptom relief and managing the underlying causes.
Dental professionals or healthcare providers may recommend various strategies to alleviate dry mouth symptoms.
These can include lifestyle modifications such as staying hydrated, avoiding caffeine and tobacco, using over-the-counter saliva substitutes or moisturising mouth sprays, and practising good oral hygiene. In some cases, prescription medications that stimulate saliva production may be prescribed.
Your healthcare provider will work with you to develop a personalised treatment plan that addresses your specific needs.
Suppose dry mouth persists even after a dental analysis. In that case, it may indicate underlying medical conditions such as diabetes, stroke, thrush (yeast infection) in the mouth, Alzheimer’s disease, autoimmune diseases like Sjogren’s syndrome, or HIV/AIDS. These conditions can contribute to dry mouth.
It is vital to seek a medical professional for a proper diagnosis and recommended treatment for your condition.
Summary
Dry mouth can significantly impact oral health and overall well-being. If you’re experiencing symptoms of dry mouth, it’s essential to consult a dental professional or healthcare provider for a proper diagnosis and personalised treatment plan.
While home remedies can provide temporary relief, addressing the root causes of persistent dry mouth is crucial for long-term oral health. Don’t let a dry mouth affect your quality of life, seek professional assistance and regain comfort and moisture.
Please note that the information provided in this article is for educational purposes only and should not substitute professional medical advice. Consult a dental professional or healthcare provider for personalised diagnosis and treatment options specific to your situation.